Helping healthcare professionals improve patients' quality of life is one of the most rewarding aspects of Sharan Saduera's job.
Sharan, a qualified dietitian, talks about her work in Nestlé Health Science and her area of expertise, tube feeding.
I trained as a dietitian 16 years ago and worked for the NHS in both a hospital and the community for six of those years. I also worked as a Home Enteral Feeding (HEF) dietitian, where all the patients on my caseload would have a feeding tube to help provide their nutrition and hydration.
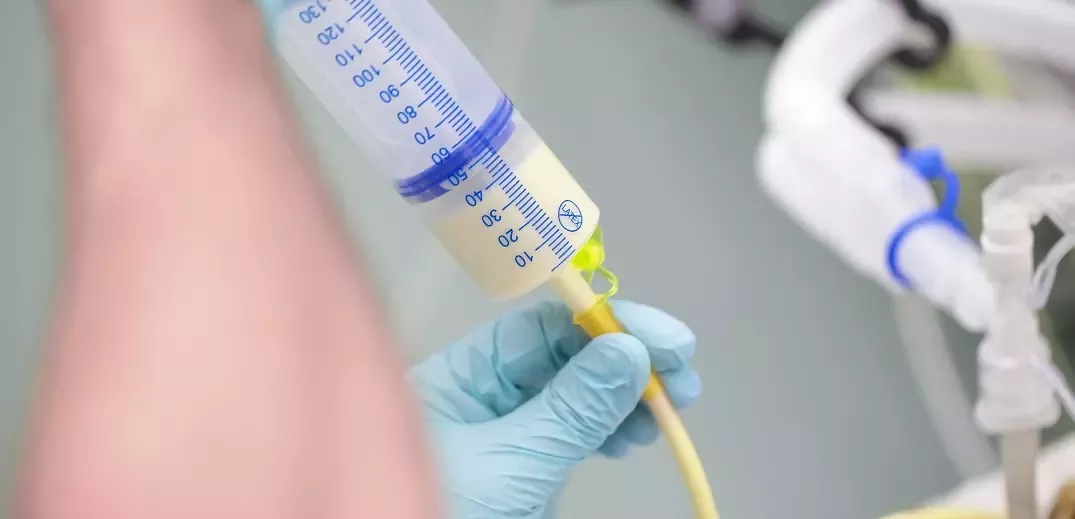
Tube feeding (also known as enteral nutrition) is where patients get their nutrition through a small plastic feeding tube which enters via the nose and into the stomach, or directly into the stomach. This may be their sole source of nutrition, or some might continue eating small amounts orally.
I specialise in gastrointestinal disease, which means helping patients to manage their conditions, whether that’s inflammatory bowel disease such as Crohn’s disease or Ulcerative Colitis. For example, an entirely liquid diet for Crohn's patients may alleviate a lot of the symptoms they are experiencing, either in the short or long term.
My job now as a medical affairs manager at Nestlé Health Science means speaking peer to peer with my dietetic colleagues in the NHS about the choices made when managing their patient's condition, often relating to Nestlé Health Science products. It can be so rewarding to hear how a change in feeding regimens can help a patient improve.
Clinical trials are set up with healthcare professionals, mainly dietitians, in the NHS to gather data and case studies around our products, in order to help share best practice with other healthcare professionals.
One of the areas we've been working on is blended diets. This is where people incorporate food into their feeding regimen - either by blending meals and administering through their tube or doing this alongside their formula - this is also known as 'bridge feeding'. Some patients, understandably, miss drinking tea or having their favourite foods or treats, so this can be a way to still enjoy them. Although food can be blended, there can sometimes be issues with tube blockages, which would mean a trip back into hospital, so it can be tricky to manage.
A recent study in children using a tube feed containing food-derived ingredients showed improvements in weight and gastrointestinal symptoms (vomiting, reflux, diarrhoea and constipation). Seeing the impact and improvements these changes in the diet can have on a patient's quality of life is what motivates me.
Dietitians always want something new; they want to keep up to date. They are continually helping us to improve our products and services by taking part in research with us and sharing their expertise - we're so grateful to them.
After all, dietitians want a solution for their patients, they want to make sure symptoms are reduced - that's the end goal. To see this happen is what makes us all, as dietitians, really happy.
I've seen the huge difference Nestlé Health Science is making, really improving the quality of life for patients, which makes me so proud.
Five things to know about tube feeding
- Tube feed formulas are a liquid that contains the energy, protein, vitamins and minerals, with or without fibre, required by the patient to meet their daily needs.
- Feeds are administered via a small plastic tube which passes either through the nose down into the stomach (nasogastric tube) or directly into the stomach via a PEG tub (Percutaneous endoscopic gastrostomy tubes).
- Tube feeds can be used on a short or long-term basis.
- Tube feeding can support babies and children, right through to older people in care homes who have a range of conditions such as a stroke which causes swallowing problems, to those with head and neck cancer.
- Although primarily tube fed, some people might still be able to have a little food and drink orally too.